Medically reviewed by: Sarah Adams, MD, OCRA Scientific Advisor
Ovarian cysts are fairly common, but that doesn’t make having them any less nerve-wracking. If you’ve been diagnosed with an ovarian cyst, it’s natural to wonder if that means you have, or are at risk of developing, ovarian cancer.
While it’s important to be vigilant when it comes to any abnormality, you should also know that having an ovarian cyst does not necessarily mean you have ovarian cancer.
It’s important to understand what cysts are, how they’re formed, and when – and how – to work with your doctor to look into them further.
As always, you should ask questions and be sure they’re answered satisfactorily. If you don’t feel heard, or suspect that your concerns are not being taken seriously, seek a second opinion.
What is an ovarian cyst?
An ovarian cyst is a fluid-filled sac or pocket that forms in the ovary or on its surface. Ovarian cysts are most common in women who have not gone through menopause because they’re often formed as part of the regular menstrual cycle. An ovarian cyst that develops after menopause should be looked into by a gynecologic oncologist, as these cysts have a higher likelihood of malignancy.
Each month before a woman has a period, the ovary grows a cyst-like structure, called a follicle. The cells lining the follicle produce the hormones progesterone and estrogen, which help to release an egg from the follicle and support possible conception. When the follicle bursts and the egg is released down the fallopian tube, this is called ovulation.
Types of Ovarian Cysts
Ovarian cysts can be classified into functional and non-functional types.
Functional cysts
Ovarian cysts that form as a result of the menstrual process are called functional cysts. These types of cysts are benign (not cancerous), and usually go away on their own within 2-3 months. Read more about functional cysts.
The two types of functional cysts are follicular cysts, which form when the follicle doesn’t release an egg, and corpus luteum cysts, which develop after ovulation and may fill with fluid or blood.
Non-functional cysts
Some ovarian cysts are not related to normal menstrual function, and may be caused by abnormal cell growth. These non-functional cysts are less common and are often benign, but they may be more difficult to distinguish from ovarian cancer based on appearance. Additional work-up may be required to make a definitive diagnosis in these cases. Read more about pathological cysts.
Examples of benign non-functional cysts include dermoid cysts (teratomas), which may contain multiple cell types; endometriomas, which often form in association with endometriosis; and cystadenomas, which are fluid-filled cysts that can grow large and sometimes cause discomfort.
How Common are Ovarian Cysts?
Ovarian cysts are very common, especially during the reproductive years. It’s estimated that 8% of premenopausal women develop cysts large enough to require treatment. Many others have smaller, functional cysts that form and resolve without ever causing symptoms or needing medical attention.
How Fast Do Ovarian Cysts Grow?
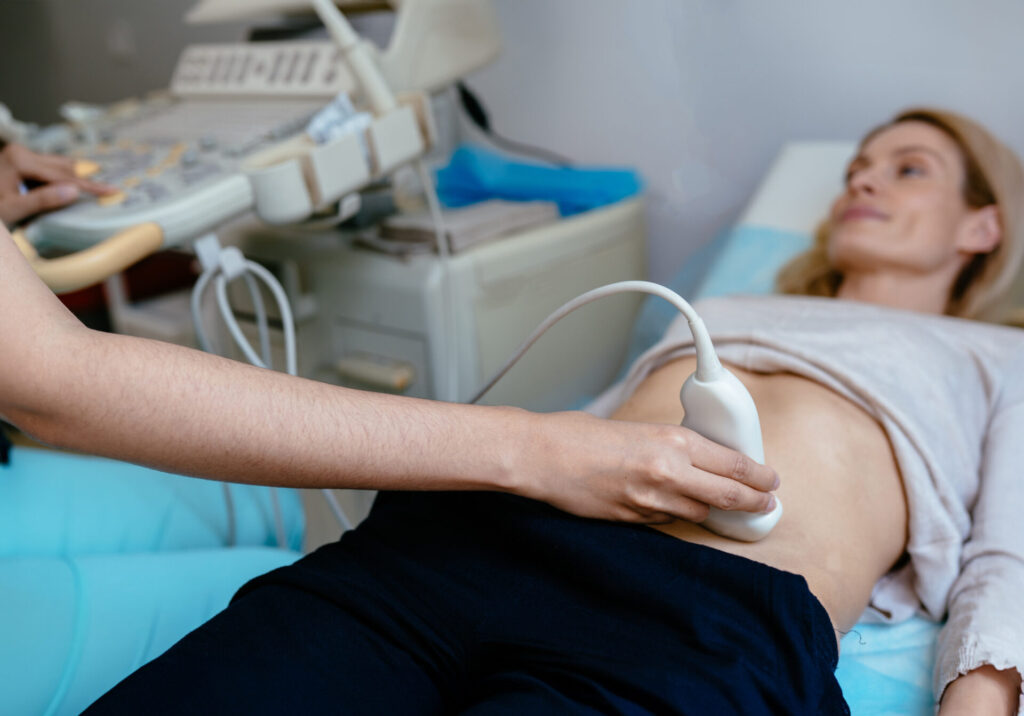
Ovarian cysts can grow at varying rates, depending on their type and individual factors. Most functional ovarian cysts are small and harmless, coming and going without an individual even realizing they are present during the childbearing years. However, some cysts can grow large. If you have questions about ovarian cysts, it’s important to consult your healthcare provider or gynecologist, who can provide advice based on your personal medical history and circumstances.
What Size of Ovarian Cyst is Considered Concerning?
A cyst’s size can be one factor in determining whether it needs further evaluation. That said, size alone doesn’t determine whether a cyst is dangerous. What matters more is the cyst’s appearance on imaging, such as whether it’s fluid-filled or contains solid areas, as well as symptoms and patient history. Your healthcare provider may recommend continued observation, additional imaging, or surgical evaluation based on these factors.
Factors Affecting Growth Rate
Several factors can impact the growth of ovarian cysts:
Type of Cyst: Functional cysts, often associated with the menstrual cycle, can grow quickly but will typically disappear on their own, without intervention. Other ovarian cyst types, like dermoid cysts and cystadenomas, may grow more slowly.
Hormonal Fluctuations: Changes in hormonal balance, often associated with the menstrual cycle or hormonal therapies, can affect cyst growth.
Monitoring Ovarian Cysts
If you have been diagnosed with an ovarian cyst, your healthcare provider will make a recommendation based on the appearance of the cyst on imaging, your age and medical history, and whether you have a family history of cancer. This may involve follow-up check-ups and ultrasounds to monitor the size and growth rate of the cyst, additional imaging with a CT or MRI, or possibly surgery for definitive diagnosis. If you are postmenopausal, or if the cyst does not resolve on its own, more frequent monitoring or surgery might be indicated.
It’s crucial to seek medical attention if you experience severe abdominal pain, fever, rapid breathing, or symptoms of shock, as these may indicate a medical emergency.
What is the Treatment for Ovarian Cysts?
Treatment for ovarian cysts depends on the type of cyst. Information that can help determine whether a cyst is functional or likely benign includes the size, composition, and symptoms associated, as well as the patient’s age and overall health. Options may include:
Monitoring: Many functional cysts resolve on their own without treatment, so your healthcare provider may suggest a period of observation with regular follow-up ultrasounds.
Surgery: Although the appearance of a cyst on imaging provides information about the likelihood that it is benign, removing a cyst so it can be evaluated by pathologists is the only way to make a definitive diagnosis. In some cases, such as when the cyst is large, doesn’t go away on its own, causes symptoms, or is suspicious for cancer, surgery may be necessary. The type of surgery will depend on several factors and may range from a cystectomy (removal of the cyst alone) to an oophorectomy (removal of the entire ovary).
How is an ovarian cyst disinguished from ovarian cancer?
Although definitive diagnosis requires surgical removal of an ovarian cyst, sometimes the symptoms a person experiences or the appearance of the cyst imaging studies can provide information that is helpful in determining the likelihood that a cyst is benign, and directing the next steps.
Symptoms: Because functional ovarian cysts don’t always produce symptoms, and may resolve on their own, many people have them and never know it. In some cases, asymptomatic cysts are first found during pelvic exams performed by a gynecologist or primary care physician. In other cases, ovarian cysts may cause symptoms that prompt people to seek medical attention. These symptoms are important to discuss with your healthcare provider to help determine next steps for work-up.
- Ovarian cysts may cause pain in the abdomen or pelvis, or pain with intercourse.
- Pressure from ovarian cysts can also be associated with bloating, changes in bowel habits, or frequent urination.
- Some ovarian cysts may be associated with irregularities in the menstrual cycle.
Appearance on imaging: Although surgical removal is required for diagnosis, the appearance of benign ovarian cysts is often different than the appearance of ovarian cancers:
- Ovarian cysts that are filled with fluid without solid areas are less likely to be cancer, particularly in young women.
- Ovarian cysts that come and go with menstrual cycles are likely benign functional cysts.
- After menopause, when the ovary stops producing follicles, the possibility that a cyst may be cancer is higher.
- Ovarian cysts that persist may require surgery for diagnosis and treatment.
- A 2019 study found that a higher percentage of complex ovarian cysts may be cancerous, estimating that among those age 50 or older, 6.5% of individuals with complex ovarian cysts may be diagnosed with ovarian cancer within 3 years. The UKCTOCS study found the risk of cancer in those with complex ovarian cysts to be .4% to 6.6%.
Are ovarian cysts painful?
Many ovarian cysts are painless and go unnoticed. However, some may cause pelvic or lower abdominal discomfort, especially if they grow large or occur around the time of ovulation. The pain may be dull and intermittent, or more noticeable during menstruation or intercourse.
Sudden sharp abdominal pain, fever and nausea can be a sign that an ovarian cyst has ruptured or twisted, and requires quick medical attention often followed by emergency surgery.
Work-up once a cyst is found
Once a mass is identified and a cyst is suspected, doctors may perform additional tests to determine whether the mass is a benign cyst or whether it could be a cancer. Most ovarian cysts are not cancerous, but some complex cysts, especially in postmenopausal individuals, may carry a higher likelihood of being malignant and warrant closer evaluation. To assess this, doctors may recommend further diagnostic steps, which may include:
- Pregnancy test: Some complications of pregnancy, like an ectopic pregnancy (a pregnancy that implants in the wrong place, usually in the fallopian tube) can look like an ovarian cyst. It is important to know if a person is pregnant to decide what additional tests are needed to evaluate an ovarian cyst.
- Blood tests: Blood tests to look for signs of infection, anemia, or tumor markers (proteins associated with some kinds of cancer) may be performed to help characterize a cyst.
- Transvaginal ultrasound: This will let a doctor see the size, shape, location, and features of an ovarian mass. A doctor may suspect an ovarian cancer, and perform additional testing, if an ultrasound indicates the mass looks solid or complex (as opposed to fluid-filled and simple), or if there is increased blood supply flowing to it.
If a doctor suspects a benign cyst after performing these tests, the next course of action in a pre-menopausal person may be to keep an eye on the cyst through more ultrasounds over the next several months to make sure it resolves and does not continue to grow. Since the risk that a cyst may be cancer is higher after menopause, additional tests may be performed in those cases.
A CA125 blood test measures a protein that is often elevated in people with ovarian cancer. A doctor may perform a CA125 if a patient is considered high risk for ovarian cancer, or if the ultrasound shows characteristics of a cancer. It’s important to note that CA125 levels are not diagnostic since they can also be elevated in noncancerous conditions, like endometriosis, uterine fibroids, and pelvic inflammatory disease.
If a doctor suspects a cancer, the patient should then be referred to a gynecologic oncologist for further follow-up. The gynecologic oncologist may or may not recommend surgery to determine if the mass is cancerous. And if it is determined to be a benign cyst, and not a cancer, you will likely be referred back to your gynecologist.
What makes some people more prone to ovarian cysts?
Different factors can predispose some people to certain types of cysts. For instance, hormonal therapy , including some drugs that promote conception, can lead to ovarian cysts. Endometriosis, pelvic infections, complications in early pregnancy, and Polycystic Ovary Syndrome can also be associated with the formation of cysts. Learn more about risk factors for ovarian cysts.
A final note on ovarian cysts:
In short, an ovarian cyst is not necessarily a cancer. It is important to review your family history, symptoms, and medications with your medical provider to determine the next steps if a cyst if found. Know the facts, and make sure you’re clear on the process that should be used to investigate suspected cysts to rule out ovarian cancer. If you feel your questions are not being answered, be your own advocate and seek another medical opinion.
Learn more about ovarian cysts:
You can find additional information on treatment, surgery, questions to ask your doctor and more in the Ovarian Cysts section of our website.



