Ovarian Cancer
Often starts in the fallopian tubes and can be hard to detect early. Learn the symptoms, types, and how it’s diagnosed and treated.
Gynecologic cancers affect the reproductive organs, including the uterus, ovaries, cervix, vagina, and vulva. An estimated 110,000 individuals will be diagnosed with gynecologic cancer in 2025. Understanding the risks, recognizing early symptoms, and getting regular screenings can make a critical difference in treatment and recovery.
Medically Reviewed By: Sarah Adams, MD, OCRA Scientific Advisor
Gynecologic cancers are not all the same. Each type begins in a different part of the reproductive system and has distinct signs, risk factors, and treatment approaches. Some, like cervical cancer, may be detected early through regular screening, while others, such as ovarian cancer, are more difficult to diagnose in early stages. Understanding the differences can help guide decisions about prevention, early detection, and care. Explore each cancer type to learn more about symptoms, treatment options, and available support.
Often starts in the fallopian tubes and can be hard to detect early. Learn the symptoms, types, and how it’s diagnosed and treated.
Highly preventable through screening and HPV vaccination. Explore symptoms, staging, and how early care can make a difference.
The most common gynecologic cancer. Learn what symptoms to watch for, who’s at risk, and how it’s treated.
A rare cancer of the uterine muscle and support tissues. Find out how it’s different from other uterine cancers and what to expect.
Vaginal cancer is uncommon, but early detection matters. Learn the signs, risk factors, and next steps for care.
A cancer affecting the outer genital area. Learn what symptoms to look for, risk factors, and how early treatment can help.
Tune in to this video presentation by Dr. David Huntsman, Professor at the University of British Columbia and the Canada Research Chair in Molecular and Genomic Pathology, for a thought-provoking exploration of what we can learn about ovarian cancer by expanding our knowledge of other gynecologic cancers.
Whether you’ve just received a diagnosis or are navigating treatment, OCRA offers resources to help guide, inform, and support you every step of the way.
You are not alone. Our Woman to Woman peer mentorship program connects gynecologic cancer patients with trained survivors for one-on-one support. We also offer weekly virtual support groups and an online forum to help you feel connected and empowered.
Looking for new treatment options? Our Clinical Trial Navigator is a free, personalized tool that helps you find trials based on your cancer type, location, and treatment history. Get matched in minutes.
Being newly diagnosed with a gynecologic cancer can raise many questions. We’re here to help you make informed decisions. Find answers about treatment, second opinions, emotional support, and how to prepare for what’s ahead.
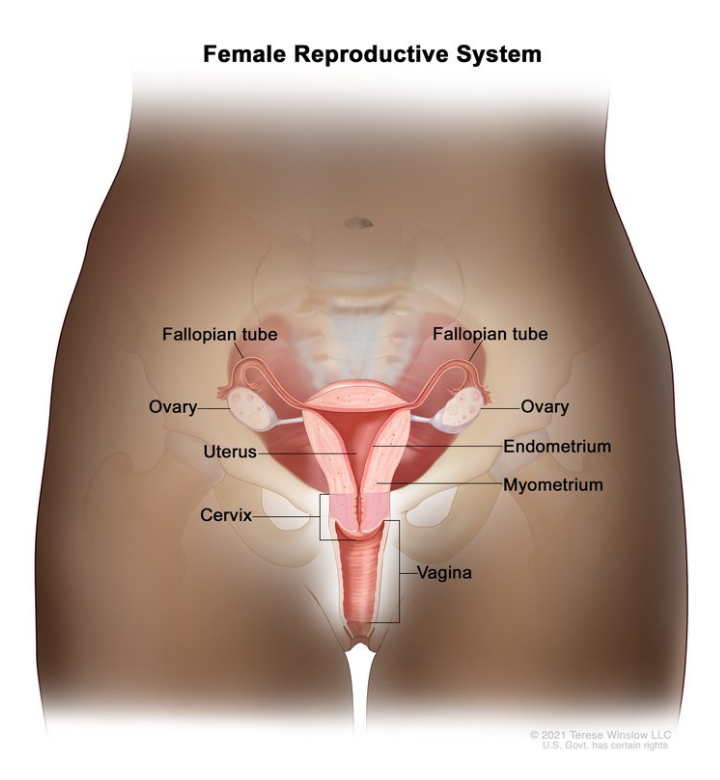
Gynecologic cancers start in a woman’s reproductive organs. The five main types include ovarian, cervical, endometrial (uterine), vaginal, and vulvar cancers. Each type is different in where it starts, how it behaves, and how it’s treated.
Gynecologic cancers are diagnosed through a combination of physical exams, medical history review, imaging tests, lab work, and tissue sampling. Diagnosis often begins with a pelvic exam and a discussion of symptoms. Depending on the cancer type, doctors may use tools such as transvaginal ultrasound, CT or MRI scans to evaluate the presence and extent of disease. Usually a biopsy or surgery is required to confirm a cancer diagnosis.
Some gynecologic cancers, like cervical cancer, can be detected early through routine screening with Pap and HPV tests. Others, like ovarian or endometrial cancer, are typically diagnosed after symptoms appear.
Some gynecologic cancers are highly preventable. Cervical cancer can often be prevented through HPV vaccination and routine screening. Many vaginal and vulvar cancers can also be prevented through HPV vaccination. Research shows that removing the fallopian tubes may prevent the most common type of ovarian cancer.
Knowing your risk factors and prevention tools, and staying aware of symptoms, can help lead to earlier detection and potentially improve outcomes.
Yes, when found early, many gynecologic cancers are highly treatable. Treatment options vary based on the cancer type and stage and may include surgery, chemotherapy, radiation, immunotherapy, or targeted therapy.
If something feels off, talk to your doctor or a gynecologic cancer specialist to get answers and take the next step in your care.

Audra Moran, President and CEO of Ovarian Cancer Research Alliance (OCRA), has been recognized as a Crain’s New York Business 2026 Notable Leader in Health Care. Crain’s annual recognition spotlights health care executives whose leadership, innovation, and community commitment set a high bar for the field. Honorees are selected based on demonstrated impact, both within … Continued

This article was updated in April 2026 to reflect NCCN’s release of the 2026 Guidelines for Uterine Cancer Patients. OCRA is a proud sponsor of the 2026 Patient Guidelines for Cervical Cancer and Uterine Cancer, and the 2025 Patient Guidelines for Ovarian. We believe ensuring access to clear, understandable information is critical. NCCN provides wonderful … Continued

On March 25, 2026, the U.S. Food and Drug Administration (FDA) approved Lifyorli (relacorilant), made by Corcept Therapeutics, in combination with Abraxane (nab-paclitaxel) for adults with platinum-resistant epithelial ovarian, fallopian tube, or primary peritoneal cancer who have received one to three prior lines of treatment, including prior Avastin (bevacizumab). The approval follows last month’s FDA … Continued
Get email updates about research news, action alerts, and ways to join the fight.